Following
are a few client case studies that will provide you an overview
of our work structure and capabilities:
Drug
Adjudication System
Drug
Adjudication System is part of an existing product for Health
Insurance System. The system is initially being built for
Adjudication of Drug Claims for Canada, Brazil, USA and South
Africa. The system is being developed on Windows 2000 with
SQL 2000 as database server, and uses for VB and C++ for front-end
clients and middle tier respectively as development platforms.
The system interfaces with other databases for getting Recipient's
information, Policy information, etc. The effort involved
in developing it is about eight person years.
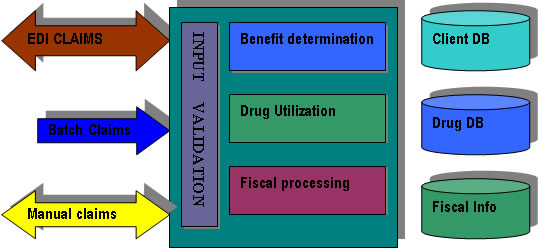
Drug
Claims can be submitted on Paper or as Electronic transmissions.
Electronic transmissions support CPhA version 3.0, NCPDP versions
3.2 and 5.0. The claims can be submitted in a batch as well.
The Physicians' prescriptions are also processed for adjudicating
the claims. There can be batch electronics submissions as
well. After performing the basic checks and validating the
inputs, the information is passed on to Benefits Determination
module to determine the eligibility, duplicate claims, validating
the Drug information, Drug eligibility, Drug plan, etc. The
system supports the ability to define exceptions to a drug
plan based on any of the drug classification parameters of
a drug. The system supports the pre-authorization, Prescriber
restrictions, days supply limits, Trial Drug processing, Maintenance
Drug processing, Treatment Protocol rules and so on.
The
system also performs Drug Utilization review, wherein various
checks are carried out. The checks include Duplicate drug,
Duplicate therapy, Refill too soon / too late, Drug to drug
interaction, Minimum / maximum daily dosage, Pediatric precaution,
Geriatric precaution, Drug to gender contraindication, Drug
to known disease contraindication, Drug to inferred disease
contraindication, Drug to allergy contraindication, Drug to
pregnancy contraindication, Drug to lactation contraindication,
and Duration of therapy. If any of the checks indicates a
severity for the usage of the Drug, the claim can be rejected.
Subsequently,
fiscal processing is carried for the claim to determine the
portion of the eligible claim amount that is payable by the
recipient. Various fiscal rules like co-pay, co-insurance,
deductible and maximums are supported. There are various variations
supported for the fiscal rules like simple, sliding, maximums,
etc. The system supports the option for automatic pro-ration
of limits based on the enrolment date of the certificate holder
or recipient. The fiscal rules can be specified in variety
of ways.
The
system supports the maintenance of multiple prices for each
drug in each province/state, for different effective periods.
Drug pricing information includes wholesale price, retail
price, BAP (best available) price, formulary (provincial or
state) price, etc. Multiple pricing rules supported by the
system include No drug pricing, Generic pricing, Mandatory
generic pricing, LCA (lowest cost alternative pricing), GCN
pricing and Therapeutic equivalent pricing. It supports definition
of different rules regarding allowable sales tax when calculating
the eligible drug cost and professional fee.
Lastly,
coordination of benefits is done. It supports the ability
to determine the primary payer for a Recipient. It supports
various mechanisms like the ability to automatically adjudicate
a claim under both the primary and secondary plan where both
the certificate and spouse are covered under the same Insurer
or ASP/PBM. It also supports the unique processing requirements
of Bill 33.
|